The beginnings of Brudy date back to 1995, when, in collaboration with the American company Omegatech, we introduced Omega-3 fatty acids in food products in Europe, such as eggs, sausages and industrial pastries. In 1997, our efforts were recognized with the Most Innovative European Product Award for eggs enriched with Omega-3, achieving sales of 60 million euros per year in Spain, Portugal and France.
From our origins in the food sector, we took a leap towards Nutraceuticals by manufacturing the first European oils rich in DHA under the Algatrium® brand. Initially, we used Schizochitrium algae oil, which we later replaced with oil extracted from fish. In 2008, we received the prestigious Health Ingredients Award Europe 2008.
With an investment of more than 10 million euros of 100% Spanish capital, we have obtained three patents worldwide for the use of Triglyceride concentrated in DHA, an achievement of which we are proud.
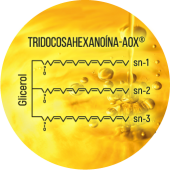
At Brudy we are not satisfied that our Triglyceride concentrated in DHA (Tridocosahexaenoina-AOX) meets the most demanding international quality standards for Omega-3. We go above and beyond, demanding that our DHA retain maximum Bioactivity. We are the only company in the world that biologically guarantees this Bioactivity through the Cellular Bioactivity Test.
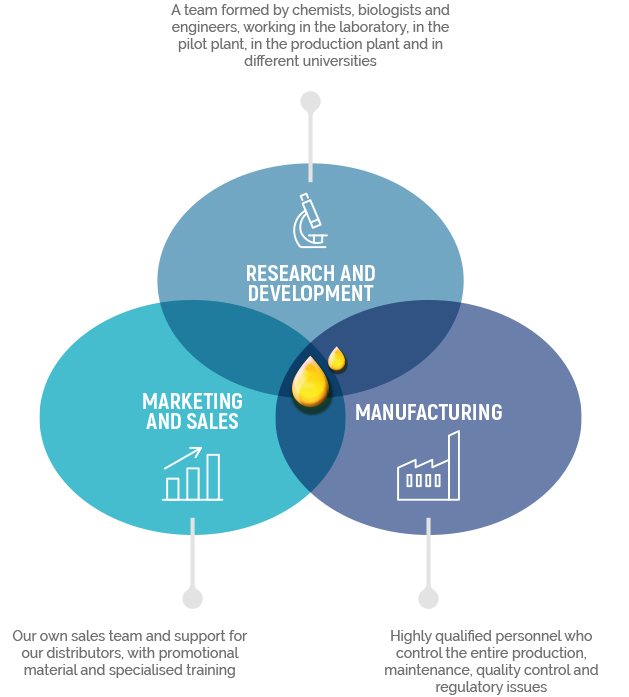
Our team:
Since 1995, the BrudyTechnology team has been driven by a passion for research and developing new products with DHA molecules derived from fish marine oil.
Our team consists of three divisions that work together to produce the highest quality oil possible. We believe that the extraction of rich marine lipids is not only a technical process, but rather an art; the art of preserving BIOACTIVITY, which sets us apart from all others in our field.
Our mission, vision and values
Mission:
We provide innovative and tailored solutions to meet current needs by addressing the global Omega-3 deficiency, aiming to improve people’s quality of life and contribute to the treatment of diseases associated with oxidative stress and inflammation.
Vision:
To become a national and international benchmark in the field of Omega-3 fatty acids, offering products in the nutritional, cosmetic, and medical device sectors.
Values:
-
Innovation and continuous improvement in our processes and products, always striving to meet the highest standards and quality expectations in the market.
-
Commitment to the health and well-being of our customers and staff, offering products that meet the needs of the nutritional, cosmetic, and healthcare markets.
-
Social and environmental responsibility, promoting sustainable practices in all our activities, such as implementing measures to prevent and reduce food waste.
-
Compliance with applicable legal and regulatory requirements, as well as with the commitments made to our clients and other stakeholders.
-
Establishment and periodic review of quality objectives, ensuring continuous improvement of our processes and quality management systems.
-
Promotion of training and awareness among our staff, fostering a culture of quality and responsibility across all areas of the company.
– Updated June 2025 –
BRUDY’s story is associated with research
on the healthy effects of omega-3
polyunsaturated fatty acids on human health
1995
Since the launch in 1995 of the first foods enriched with Omega-3 in Europe (eggs and milk), in 1998 began with the development chemistry of Omega-3 molecules for human medical applications. In 2001 we start laboratory enzymatic production.
2001
Launch of the first DHA 70% triglyceride;
a high concentration Omega-3 obtained
from fish.

2010
In 2010 the commercial division BRUDYLAB is created, which begins the commercialization of Food Supplements and Food for Special Medical Purposes for eye care, to promote fetal and neonatal neurodevelopment, liver and immune care, and starting the clinical research in all these areas.

2012
As of 2012, BRUDY expands its sales to Japan and Russia.

2015
In 2015 the patent is approved with a coverage for 90 countries (Asia, Europe, USA, Oceania) for ophthalmic use, in the central nervous system and in Oncology, and since then we began to publish the first clinical research results in the ocular area: dry eye, glaucoma, diabetic retinopathy, anterior uveitis, but also in sport, fertility, and we started the research into new areas such as hepatology, neuropediatrics (ADHD), obstetrics and neonatology.

2017
In 2017 the approval of the patent isratified by European courts, and begins the expansion to Mexico, Switzerland, Greece, Czech and Slovak Republics.

2019
In 2019 Italy and Brazil join.

2010-2022
In 2015 the patent is approved with a coverage for 90 countries (Asia, Europe, USA, Oceania) for ophthalmic use, in the central nervous system and in Oncology, and since then we began to publish the first clinical research results in the ocular area: dry eye, glaucoma, diabetic retinopathy, anterior uveitis, but also in sport, fertility, and we started the research into new areas such as hepatology, neuropediatrics (ADHD), obstetrics and neonatology.

27 years dedicated to research on the healthy effects of DHA, and at the service of human health.

